Empower Your Loved One: Fight Diabetes and Reclaim Their Golden Years
Have you ever watched a TV program or film where the characters comment: “If you eat that your foot will foot off?”

Well, it can get that serious but there’s a lot that can be done before it reaches that level.
Diabetes becomes increasingly common as we age, impacting over 1 in 4 seniors.
The prevalence of diabetes rises steadily after age 45, doubling every decade. Yeah, that is scary to think about.
With age, the body becomes less responsive to the hormone insulin, which transports glucose from the bloodstream into cells. This condition, known as insulin resistance, causes high blood sugar and type 2 diabetes.
However, with diligent lifestyle management and proper medication, older adults can control diabetes and reduce the risks of serious complications.
Table of Contents
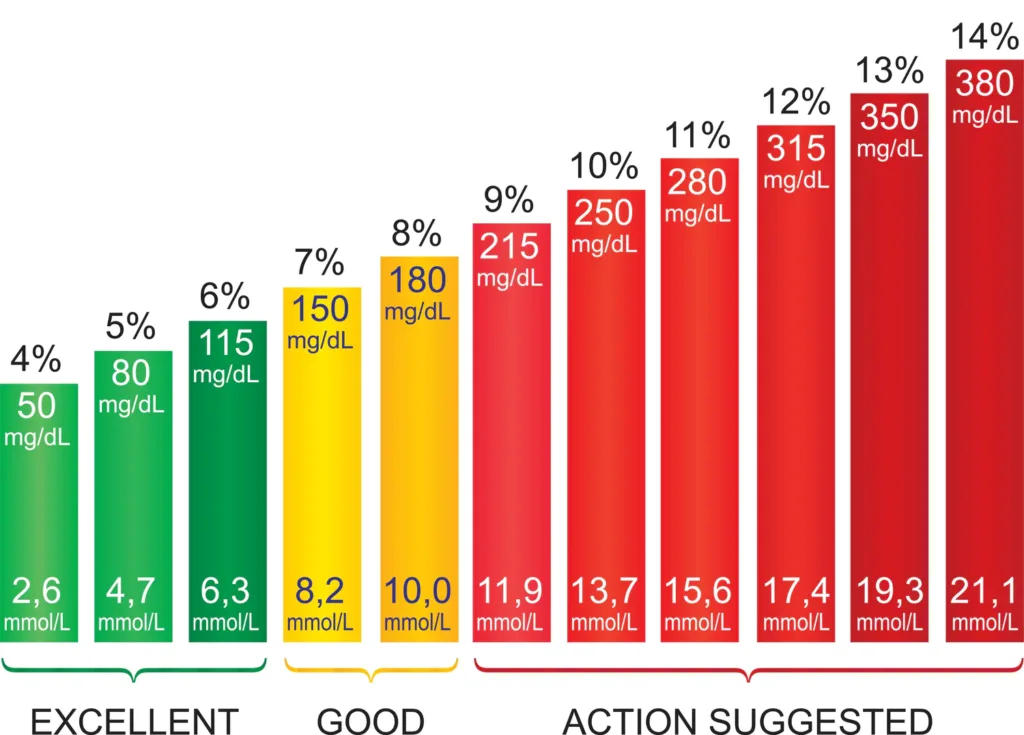
Assessing for Diabetes – A1C goals by age chart
What is A12?
Doctors utilize a blood test called the A1C to assess average blood sugar levels over 3 months.
The American Diabetes Association recommends the following A1C goals based on age:
- For those under age 65, aim for an A1C under 7%
- For those between ages 65-75, aim for an A1C under 7.5%
- For those over age 75, aim for an A1C under 8%
Higher A1C targets are set for older adults due to the increased risks of hypoglycemia in seniors.
However, these are general guidelines only. Be sure to discuss personalized A1C goals with your physician based on your health status and risk factors.
Tighter control may be advised for younger or healthier seniors. Getting your A1C tested every 6 months helps monitor if treatment targets are being met.
Monitoring Diabetes
Blood glucose testing a.k.a blood sugar testing is done to get real-time snapshots of current blood sugar levels.
A finger prick sample of blood is placed on a test strip inserted in a glucose meter, which provides the reading in mg/dL.
Testing is done when fasting, before meals, and 1-2 hours after meals to identify fluctuations.
These instant readings differ from the A1C test, which measures average blood sugar over the prior 2-3 months by detecting what percentage of hemoglobin is glycated (coated with sugar).
While glucose testing shows short-term levels, the A1C provides the bigger picture of overall glucose control.
To get an accurate blood glucose level (BGL), wash your hands with soap and water before pricking the side of the fingertip with a lancing device. Apply the drop of blood to the test strip according to meter instructions.
Prevalence and Risk Factors
Several factors make seniors especially vulnerable to developing type 2 diabetes:
- Age – The pancreas produces less insulin, and cells become resistant to it.
- Weight – Excess fatty tissue contributes to insulin resistance.
- Inactivity – Regular exercise helps regulate glucose levels.
- Diet – Sugary and high glycemic index foods spike blood sugar.
- Genetics – Family history strongly predicts diabetes risk.
- Race – Greater prevalence in Hispanic, African-American, and Native American populations.
- Hypertension – Makes the body less able to regulate glucose.
- Prediabetes – Blood sugar levels are elevated but not yet diabetic. Slowing progression is crucial.
Signs and Symptoms
The early signs of diabetes can be subtle. Monitor for:
- Increased thirst and frequent urination – High glucose spills into urine pulling fluid from tissues.
- Fatigue – Cells deprived of glucose for energy.
- Blurry vision – Fluid pulls from the eyes.
- Slow healing cuts/bruises – Circulation is impaired.
- Tingling hands/feet – Nerve damage from high glucose.
Lab tests revealing an A1C over 6.5%, fasting blood sugar over 126 mg/dL, or random glucose over 200 mg/dL confirm diabetes. Getting tested at least every 3 years after age 45 is recommended.
Dangers of Uncontrolled Diabetes
Chronically high blood sugar damages nerves, blood vessels, and vital organs. Major complications include:
- Heart and vascular disease – 2-4 times higher risk of heart attack or stroke.
- Nerve damage (neuropathy) – Numbs and pains especially in the feet.
- Kidney disease (nephropathy) – Leading cause of kidney failure requiring dialysis.
- Eye damage (retinopathy) – Leads to blindness.
- Foot damage – Poor circulation and sensation results in ulcers, infections, and even amputation.
- Cognitive impairment – Linked to vascular dementia and Alzheimer’s disease.
Diabetes Management Strategies
Controlling blood sugar levels prevents or slows diabetes complications. Management includes:
- Monitoring blood sugar – Using a glucose meter to track levels before meals and at bedtime.
- Medications – Oral meds or injectable insulin help lower blood glucose when needed.
- Nutrition – Eating small, frequent meals with nutrient-rich carbohydrate sources like vegetables, fruits, beans, and whole grains.
- Exercise – Activity sensitizes the body to insulin and lowers glucose. Aim for 150 minutes per week.
- Weight management – Even losing 5-10% of body weight can improve diabetes control.
- Foot care – Inspecting feet daily and wearing proper footwear prevents sores and infections, see a podiatrist for a full assessment.
- Eye exams – Annual retinal screenings check for damage and deterioration of the eyes.
- Blood pressure control – Maintaining readings below 140/90 mmHg reduces risks.
- Cholesterol management – Keeping LDL levels below 100 avoids circulatory damage.
- Smoking cessation – Smoking restricts blood flow and injury-proofs vessels.
With diligent self-care, frequent monitoring, proper medical treatment, and lifestyle modifications, seniors can manage diabetes while maintaining an active, healthy life.

Supporting Care of Diabetes
Caring family members can assist with managing diabetes through useful tools and equipment like:
- Blood glucose meter – Choose an easy-to-use model with a large display.
- Continuous glucose monitor – Wearable sensors provide 24/7 glucose readings.
- Insulin pens – Prefilled pens simplify injecting insulin.
- Insulin pump – Automatically delivers insulin throughout the day.
- Compression socks – Improves circulation in feet.
- Foot spa massager – Promotes circulation and relaxation.
- Nutrition apps – Helps count carbs and log food intake.
- Food scale – Measures proper serving sizes.
- Prepared meal delivery – Healthy, diabetic-friendly meals.
Providing devices that make monitoring and medications easier demonstrates your commitment to helping them manage their condition.
Supporting a Loved One with Diabetes
Caring for an aging parent or grandparent with diabetes poses challenges. Provide support through:
- Learning about the disease – Increase knowledge so you can discuss it meaningfully.
- Helping monitor blood sugar – Record levels to identify patterns.
- Going to medical appointments – Take notes and ask questions.
- Assisting with medications – Set reminders and organize pills.
- Preparing healthy meals – Cook nutritious foods that align with dietary needs.
- Encouraging activity – Going on walks together makes fitness more social.
- Reducing risks – Help declutter to avoid falls, treat calluses, massage feet, and quit smoking together.
- Providing technology aids – Large display glucose monitors, teach video calling.
With understanding and support, people with diabetes can thrive. Your assistance makes their self-care journey easier.
Giving gifts like large-display glucose monitors, compression socks, and meal delivery shows you are invested in helping control your diabetes.
Your support motivates their self-care.
Final Thoughts: Empowering You and Your Loved One on the Journey
We understand. Watching a loved one navigate diabetes can be overwhelming. The constant monitoring, medication, and lifestyle changes can feel like an uphill battle. But remember, you’re not alone in this.
This guide equips you with knowledge, but remember, it’s just the beginning. Seek personalized advice from healthcare professionals who can tailor a plan to your loved one’s unique needs.
Empowerment is key. Encourage your loved one to participate in their own care. Work together to set realistic goals, celebrate small victories, and find healthy habits they enjoy.
Technology can be your ally. Explore tools like glucose monitors, apps, and meal delivery services to simplify management.
Don’t underestimate the power of connection. Support groups, therapy, and open communication can ease the emotional burden and foster a sense of shared purpose.
Remember, managing diabetes is a marathon, not a sprint. There will be setbacks, but with compassion, patience, and unwavering support, you can both reclaim control and create a fulfilling future together.
Here are some additional resources to empower you on your journey:
- The American Diabetes Association
- The National Institute of Diabetes and Digestive and Kidney Diseases https://www.niddk.nih.gov/health-information/diabetes
- The National Council on Aging
You’ve got this. Now go out there and empower yourselves!







